Original Articles: 2023 Vol: 15 Issue: 3
Evaluating Guideline Directed Medical Therapy (GDMT) in Yemeni��?s Patients with Heart Failure
Ali Alyahawi1*, Khalid Al-Adeeb2, Abdulsalam Halboup3, Ayed Al Shammari4
1Department of Medical Sciences, Saba University, Sana’a, Yemen
2Department of Medical Sciences, University of Science and Technology Hospital, Sana’a, Yemen
3Department of Clinical Pharmacy and Pharmacy Practice, University of Science and Technology, Sana’a, Yemen
4Department of Clinical Pharmacy and Pharmacy Practice, Kuwait University, Kuwait City, Kuwait
Received: 22-Dec-2022, Manuscript No. JOCPR-22-84508; Editor assigned: 26-Dec-2022, JOCPR-22-84508 (PQ); Reviewed: 09-Jan-2023, QC No. JOCPR-22-84508; Revised: 13-Mar-2023, Manuscript No. JOCPR-22-84508 (R); Published: 20-Mar-2023
Abstract
Background: Heart failure is a multi-faceted and life threating syndrome. In the management of CHF, a gap between Guideline Directed Medical Therapy (GDMT) and actual practice has been reported. An increase in the prevalence of co-morbid conditions and risk factors, such as increased Body Mass Index (BMI), metabolic syndrome and cigarette smoking may be some of the reasons behind the increased prevalence of HF. Aims of the study: The aims of this study are to discover the behavior of Yemeni cardiologists in treating patients with HF regarding new guideline.
Materials and Methods: This prospective study was performed at several cardiology clinics and centers in Sanaa city. Patients’ profile and prescriptions were used to collect the data by interviewing the patients and reviewing their prescriptions. A total of 177 patients with the 15 cardiology specialists and consultants were included in the current study. All data analyzed using SPSS statistics version 21.0.
Results: We found a low percentage (30.1%) of the patients were prescribed the optimum guideline directed medical therapy and the low rate of ARNi (30.1%) and SGLT2i (34.1%) prescription indicate low implication of 2022 HF guideline in Yemeni patients.
Conclusion: Yemeni patients need more help to benefit them from the guideline like more education and clinical pharmacy engagement in the treatment and telemedicine.
Keywords
ARNi; GDMT; Guideline; Heart failure; SGLT2i
Introduction
Heart Failure (HF) is a major health problem worldwide, which accounts for 1%-2% of all hospital admissions with mortality ranging from 5% to 40% and a fivefold increased risk of death compared to the general population. It is the major cause of hospitalization in older people. Hospitalization due to HF increases healthcare resource utilization, as it accounts for more than half of total healthcare costs [1].
Heart Failure (HF) is a complex pathophysiological state caused by structural and functional defects in myocardium resulting in impairment of ventricular filling or ejection of blood [2,3].
The classification system, known as the New York Heart Association (NYHA) functional classification, places the patient with heart failure into one of four categories as:
• Class I: No limitation to physical activity; regular physical activity does no longer cause symptoms.
• Class II: Slight barriers to physical activity; regular physical activity results in HF symptoms.
• Class III: Marked barriers of physical activity; the sufferers are relaxed at rest, however less than normal activity reasons symptoms of HF.
• Class IV: Not able to hold on any physical interest without HF symptoms or have symptoms when at rest.
The HF stages classified by the AHA and ACC are different than NYHA functional classifications of heart failure, ACC/AHA heart failure classification is described by using the following four stages:
• Stage A: High threat of heart failure, however no structural heart disorder or symptoms of heart failure (pre-heart failure).
• Stage B: Structural heart disease, however no symptoms of heart failure.
• Stage C: Structural heart disorder and marked limitation in activity due to symptom.
• Stage D: Severe limitations requiring specialized interventions.
An increase in percent of co-morbid diseases and risk elements along with elevated Body Mass Index (BMI), metabolic syndrome, apoB/apoA-I ratio and cigarette smoking can be a number of the reasons behind the elevated occurrence of HF [4].
The Acute Decompensated Heart Failure (ADHF) is the most common form of heart failure that accounts for approximately 80% of heart failure associated hospitalizations. The common reasons of ADHF consist of non-adherence to drugs or nutritional restrictions, uncontrolled blood pressure, ACS; dysrhythmia/arrhythmias; COPD exacerbation, alcohol intoxication or excess, thyroid disorders and other iatrogenic situations; all directly or not directly main to the development of the underlying disorder [5].
The B-type Natriuretic Peptide (BNP) degree is a robust predictor of threat of loss of life and cardiovascular events in patients formerly diagnosed with heart failure or cardiac disorder. It’s far to be remembered that increased BNP degrees have additionally been related to renal failure, pulmonary embolism, pulmonary hypertension and persistent hypoxia even as obese and obese people have particularly lower BNP degrees [6].
Identifying the specific cause of HF is crucial, due to the fact situations that reason HF might also require disorder specific treatment plans. The major goals of treatment in heart failure are:
• To improve prognosis and decrease mortality and
• To alleviate symptoms and reduce morbidity via reversing or slowing the cardiac and peripheral disorder.
For in-medical institution patients, in addition to the above goals, other goals of therapy are:
• To reduce the period of stay and next readmission
• To prevent organ system damage
• To correctly manage the co-morbidities which can contribute to bad diagnosis [7].
The 2022 AHA/ACC/HFSA guideline for the management of heart failure presents suggestions based totally on current evidence for the treatment of these patients. The suggestions present evidence based totally approach to managing sufferers with heart failure, with the purpose to enhance best of care and align with patients’ interests. The effectiveness of Angiotensin Converting Enzyme (ACE) inhibitors and b-blockers in enhancing the symptoms and prognosis of heart failure is mentioned. According to the 2022 heart failure guideline, new drug therapy in stage CHF, consisting of Sodium Glucose cotransporter-2 inhibitors (SGLT2i) and Angiotensin Receptor-Neprilysin inhibitors (ARNi) are well tested [8].
The updated guidelines make several evidence based recommendations regarding pharmacological approaches to prevent or postpone the onset of HF. Mainly the management of hypertension is given increased prominence and should be treated as per the latest clinical guidelines [9].
The 2022 AHA/ACC/HFSA guideline for the management of heart failure provides recommendations applicable to patients with heart failure as:
• ACEi or ARBs are the first line therapies recommended for all patients with CAD, regardless of HF status and in all patients with asymptomatic LV systolic dysfunction and the dose should titrate up to the maximum tolerated evidence based doses. The routine combination of ACEi, ARB and MRA is not recommended and may cause more symptomatic hypotension and worsening renal function. Angiotensin Receptor Neprilysin Inhibitor (ARNI) sacubitril/valsartan was approved by FAD in 2015 in patients with symptomatic HF.
• Beta blockers: In patients with HFrEF, with current or previous symptoms, use of 1 of the 3 beta blockers proven to reduce mortality (e.g. bisoprolol, carvedilol, sustained release metoprolol succinate) is recommended to reduce mortality and hospitalizations.
• Mineralocorticoid Receptor Antagonists (MRAs): In patients with HFrEF and NYHA class II to IV symptoms, an MRA (spironolactone or eplerenone) is recommended to reduce morbidity and mortality, if eGFR is >30 mL/min/1.73 m2 and serum potassium is <5.0 mEq/L. Careful monitoring of potassium, renal function and diuretic dosing should be performed at initiation and closely monitored thereafter to minimize risk of hyperkalemia and renal insufficiency.
• Nitrates plus hydralazine: It decreases mortality and morbidity in HFrEF among African Americans with NYHA class III-IV HF receiving Optimal Medical Therapy (OMT) with ACEi and beta-blockers.
• Aspirin and statin for ischemic HF.
• Ivabradine was approved by FAD in 2015 to reduce the risk of HF hospitalization. It is indicated in stable, symptomatic patients with chronic HFrEF.
• Digoxin: It can decrease hospitalization of HFrEF, but it does not improve survival.
• Sodium-Glucose cotransporter 2 inhibitor (SGLT2i): SGLT2i are recommended to reduce hospitalization for HF and cardiovascular mortality, irrespective of the presence of type 2 diabetes. SGLT2i are the first class of glucose lowering agents to receive approval from the FDA for the treatment of HFrEF.
In Yemen, the extent to which the guidelines for the treatment of heart failure are followed currently unclear. So, the aims of this study are to discover the behavior of Yemeni consultants in treating Yemeni patients with HF regarding new guidelines recommendations.
MATERIALS AND METHODS
Study design and location
This is a prospective cross sectional study; a validated questionnaire was distributed in several cardiology clinics and centers in Sanaa city. The cardiology centers of Al-Thawra hospital, Lebanon hospital, university of science and technology hospital, Dr. Abdulkader Almutawakel hospital and different cariology clinics were included. The previous cardiac centers and cariology clinics were conviniently selected from public and private sectors to ensure inclusion of all entities of the yemeni society. The study was conducted from March 2022 to August 2022.
Sample size and sampling method
All patients coming from different yemeni cities with HF who were followed up by the 15 cardiology specialists and consultants were interviewed by trained 6th year clinical pharmacy students. A total of 199 patients were interviewd during the study period using convenience sampling method.
Inclusion and exclusion criteria
All patients with heart failure who attended to cardiac centers and clinics and had echo result were included. Critically ill patients in the ICU, those without EF results and those who refused to participate were exluded from the study.
Study tools
Tow questionnaires were used in this study, one for the patients and another one for the cardiology physicians. Patients’ questionnaire consist of three parts. The first part , including patients’s demographic data, diagnostic data and medications data; some questions were inserted as yes or no questions, others as multiple choices and the others opened questions,whereas the specialist questionnaire consist of multiple choices only.
Data collection
Clinical pharmacy students in the final year (6th year of pharmacy) were chosen and trained by a supervisor. Then the invistigators were divided into four groups and distributed among four cardiac centers, including Al-Thawra hospital, Lebanon hospital, science and technology hospital and Dr. Abdulkader Almutawakel hospital then they distributed among several cardiology clinics. The data were collected by intervewing the patients right after having a prescription from their physicians. All cardiology physicians who were visited by the same investigators to the cardiac centers and clinics and a prevalidated questionnaire was handed to them. After answering all questionnare parts, it was collected by the investigators.
Statstical analysis
Categorical variables were represented as frequency and percentage. Kolmogorov-Smirnov was used to assess the normality of data distribution. The p-value was >0.05, showing normal distribution of the data. All data were analyzed using SPSS Statistics version 21.0 for Windows® (IBM Corp., Armonk, NY, USA). Statistical differences among groups were evaluated using Pearson’s chi-squared test. A p-value <0.05 was considered statistically significant.
RESULTS
Sociodemographic data of participants
A total of 22 patients were excluded during statistical analysis because of missing information and 177 patients with heart failure were included in the final analysis. The majority of patients which represented about (75.6%) were male and (24.4%) were female. Regarding age, the highest percentage of patients (55.7%) was in the age below 55 years old. Patients that have work were represented about (58.6%) of the patients.
Khat chewing patients were about 71.3%, however, (13.3%) of them had stopped chewing khat. Patients who are currently taking Shamma represented about (14.5%) of the patients and those who had stopped taking it were (7.9%) of the patients. Regarding cigarette smoking, (34.5%) of the patients were smokers and (23.0%) were past smokers. Table 1 illustrated the mentioned sociodemographic data.
| Variables | N | % | |
|---|---|---|---|
| Age | ≤ 55 years | 98 | 55.7 |
| > 55 years | 78 | 44.3 | |
| Gender | Male | 133 | 75.6 |
| Female | 43 | 24.4 | |
| Have work | Yes | 68 | 58.6 |
| No | 48 | 41.4 | |
| Khat chewing | Yes | 104 | 71.3 |
| No | 23 | 15.3 | |
| In the past | 20 | 13.3 | |
| Shamma | Yes | 22 | 14.5 |
| No | 118 | 77.6 | |
| In the past | 12 | 7.9 | |
| Cigarette smoking | Yes | 49 | 34.5 |
| No | 63 | 42.6 | |
| Past smoker | 34 | 23.0 | |
Table 1: Sociodemographic data of participants.
Participant’s characteristics
According to the study results, echo results were (71.5%) HFrEF, (14.5%) HFmrEF and (14%) HFpEF (Table 2).
| Type | No. of patients | Percent of patients (%) |
|---|---|---|
| HFrEF | 123 | -71.5 |
| HFmrEF | 25 | -14.5 |
| HFpEF | 24 | -14 |
Table 2: Participant’s characteristics.
In the present study, the cardiac enzymes levels were elevated in about 78.6% of the patients. Serum creatinine was abnormal in about (46.3%) of the patients and blood pressure was uncontrolled in (49.4%) of the patients. These values are summarized in Table 3.
| Test | Normal | High |
|---|---|---|
| Cardiac enzymes | 78.60% | 21.40% |
| Blood pressure | 50.60% | 49.40% |
| Creatinine | 53.70% | 46.30% |
Table 3: Summarizes the values of the tests.
The study findings showed that 84.75% of the patients have comorbidities and 65.3% of whom were experiencing less than 3 morbidities and 34.7% of whom were experiencing three morbidities or more (Table 4).
| Comorbidity | No. of patients | Percent of patients (%) |
|---|---|---|
| Presence of comorbidities | 150 | 84.75 |
| ≤ 2 comorbidities | 115 | 65.3 |
| ≥ 3 comorbidities | 61 | 34.7 |
Table 4: The presence and number of comorbidities.
In the current study, the common comorbidities among patients with HF were: HTN, DM, AF, IHD, COPD and some patients had both HTN and DM. The number and percentage of patients that had each comorbidity are illustrated in Table 5.
| Comorbidity | No. of patients | Percent of patients (%) |
|---|---|---|
| HTN | 92 | 52.3 |
| DM | 75 | 42.6 |
| HTN and DM | 58 | 33 |
| COPD | 16 | 9.1 |
| AF | 3 | 1.7 |
| IHD | 35 | 19.9 |
| Others | 37 | 21 |
Table 5: Common comorbidities among patients.
Additionally, 90.4% of the patients were on medications other than HF medications. The most of the study patients (35.9%) were diagnosed as having HF recently. 63.2% of the study patients said that the cost of the medications affects the adherence. 49.0% of the patients were educated by the doctors about the important things regarding medications.
Most of patients (68.7%) visited the cardiologists in the last 3 months and (63.1%) don’t have additional contact with the cardiologist.
Medication results
According to the medication used by the patients, about 30.1% of the patients were on the optimum GDMT. The percentage of patients who were using ACEIs/ARBs was 71.0%; those who were using BB were about 83.4%. In addition, MRA was prescribed for 38.7% of patients, diuretics were used in 90.3% of the patients, SGLT2i were taken by 34.1% of the patients, Valsartan/Sacubitril was present in the prescription of 30.1% of the patients, digoxin was prescribed for 33.0% of them and Ivabradine was taken by 10.2% of patients (Table 6).
| Medication taken | No. of patients | Percent of patients (%) |
|---|---|---|
| ACEIs/ARBs | 125 | 71.0 |
| BB | 146 | 83.4 |
| MRA | 67 | 38.7 |
| Diuretics | 159 | 90.3 |
| Ivabradine | 18 | 10.2 |
| Digoxin | 58 | 33.0 |
| Valsartan/Sacubitril | 53 | 30.1 |
| SGLT2i | 60 | 34.1 |
Table 6: Medication used by the patients.
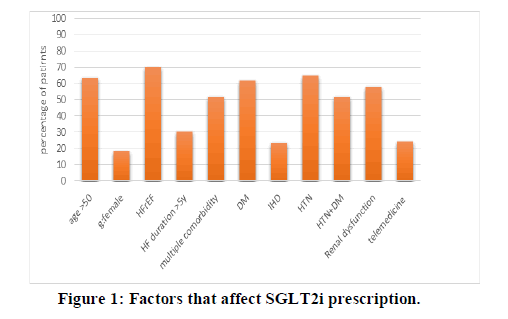
SGLT2I prescription: Most of the patients (63.3%) on SGLT2I prescription were above 50 years old and 81.7% of them were males and percent of comorbid patients with DM, IHD, HTN and renal dysfunction were 61.7%, 23.3%, 65.0% and 57.8%; respectively. There was significant association (P-value <0.05) between using of SGLT2I and number of comorbidities; DM, HTN, HTN with DM and additional contact with physicians (Figure 1).
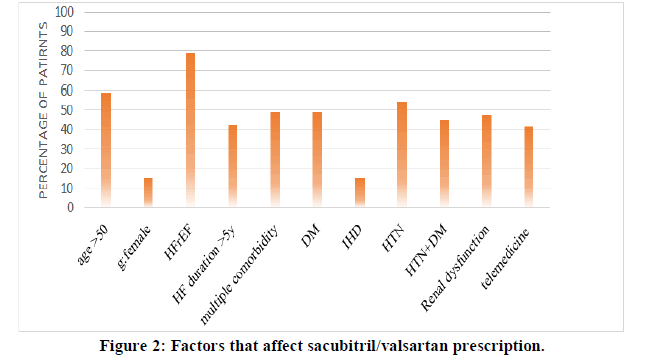
Sacubitril/Valsartan prescription: Most of the prescribed patients 58.5% were above 50 years and 84.9% of them are males. In addition, the percent of comorbid patients with DM, IHD, HTN and renal dysfunction were 49.1%, 15.1%, 54.7% and 47.7%; respectively. There was significant association (P-value <0.05) between using of valsartan-sacubitril and number of comorbidities and HTN (Figure 2).
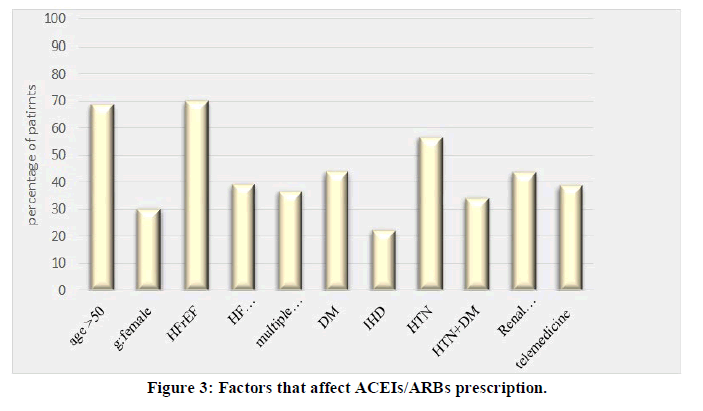
ACEIs/ARBs prescription: Most of the prescribed patients 68.8% were above 50 years and most of them were males 69.6%. Also, the percent of comorbid patients with DM, IHD, HTN and renal dysfunction were 44.0%, 22.4%, 56.8% and 43.8%; respectively. There was significant association (P value <0.05) between using of ACEIs/ARBs and gender (Figure 3).
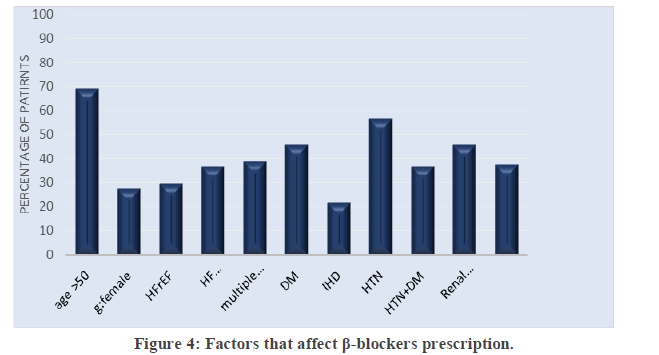
β-blockers prescription: Most of the prescribed patients 69.2% were above 50 years and most of them were males 72.6%. The percent of comorbid patients with DM, IHD, HTN and renal dysfunction were 45.9%, 21.9%, 56.8% and 45.8%; respectively. There was significant association (P value <0.05) between using of β-blockers and age patients, number of comorbidities, HTN, HTN with DM and additional contact with physicians (Figure 4).
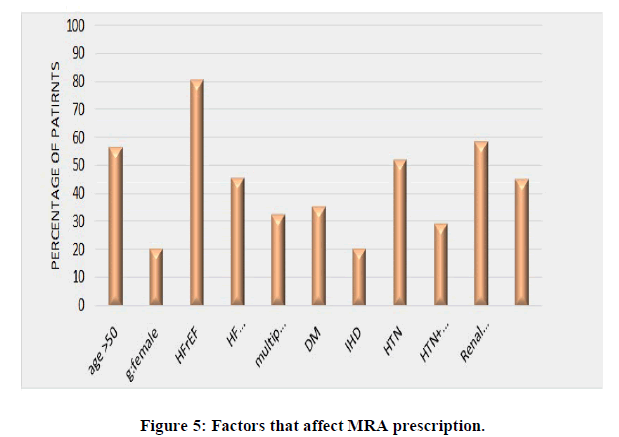
MRA prescription: Most of the prescribed patients 56.7% were above 50 years and most of them were males 79.1% and the percent of comorbid patients with DM, IHD, HTN and renal dysfunction were 35.8%, 20.9%, 52.2% and 58.8%; respectively. There was significant association (P-value <0.05) between using MRA and HFrEF, serum creatinine level and additional contact with physicians (Figure 5).
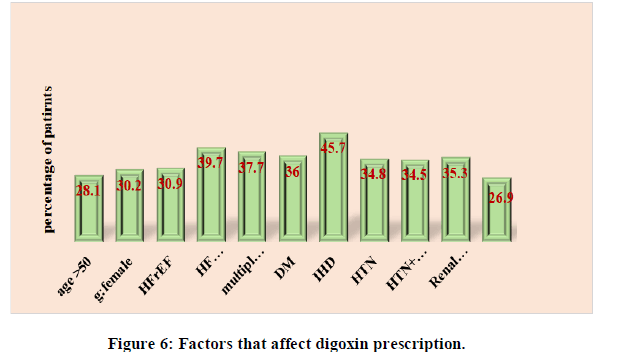
Digoxin prescription: Most of the prescribed patients 28.1% were below 50 years and most of them were males 33.8% and the percent of comorbid patients with DM, IHD, HTN and renal dysfunction were 36.0%, 45.7%, 34.8%, and 35.3%; respectively. There was no significant association between using digoxin and patient risk factors (Figure 6).
Physician’s questionnaire results
Adopting guidelines: Most of the cardiologists (60.0%) adopted to the HF guideline during practice and 60.0% of them reported that when they implemented guideline during the practice, the patients clearly improved.
Patients’ adherence: The majority 60% of physicians reported that 75% of patients use the medications as prescribed. However, 53% of the physicians said that only 50% of patient obeyed their instructions.
The importance of clinical pharmacists: The majority of physicians, which represented about (93.3%), agreed on the importance of involving clinical pharmacist in HF management.
Causes of treatment failure: All physicians agreed that shammah is a major cause of treatment failure when treating patients with heart failure, and 93.3% of physicians agreed that Khat and lack of follow up are considered major causes of treatment failure. Responses about the other causes were illustrated in the table below (Table 7).
| Cause of treatment failure | No. of physicians agreed | Percent of physician agreed |
|---|---|---|
| Shammah | 15 | 100% |
| Khat | 14 | 93.3% |
| Follow up | 14 | 93.3% |
| Knowledge | 13 | 86.7% |
| Comorbidity | 12 | 80% |
| cost of medication | 13 | 86.70% |
| cost of investigation | 12 | 80% |
| Drugs availability | 9 | 60% |
| Dose related | 11 | 73.3% |
Table 7: The responses of physician about the causes of treatment failure.
Furthermore, most of the physicians (73.3%) have read 2022 HF guideline and 33.3% of them preferred to treat their patients as the guideline regardless to other factors. Finally, when the investigators asked the physicians about the cost effectiveness in the adherence for new guideline in Yemeni patients, 41.7% of them said they can’t tolerate it [10].
DISCUSSION
This study aimed to evaluate behavior of the consultants with respect to GDMT. We found a low percentage (30.1%) of the patients was prescribed the optimum GDMT (the four drugs that all patients with HF should take ACEI/ARB/ARNI, βB, MRA, SGLT2I). Guidelines are intended to define practices meeting the need of patients in most but not all circumstances and shouldn’t replace clinical judgment and this correspond with (60%) of consultant answers that they can mostly apply guideline in Yemeni people. The most patients have not prescribed this optimum GDMT for these reasons:
• Most of them suffer from medication cost (80.2%) of patients.
• Presence of comorbid disease in (84.75%) of patients which is DM, COPD, AF, IHD, renal dysfunction and others with percentages (42.6%), (9.1%), (1.7%), (19.9%), (46.3%), (21%) respectively and (34.2%) of patients have multiple comorbidities.
• 90.4% of patients use medications other than HF medications.
• 41.7% of consultants claim they can’t tolerate it.
• The last reason is presence of factors that increase deterioration of the disease which is (71.3%) of patients is khat chewers, (14.5%) of patients use shammah, (34.5% of patients) is cigarette smokers.
• 49% of patients claim that consultant consult them about important things only and (50% of patients) not totally adherent with adherence level (75%). Comparison with Michael A Sienman study which resulted in the reasons is co-management with other clinicians (32%-35%) of patients, patient preference and nonadherence (15%-24%) and clinician belief that the medication is not indicated in the patient (12%-20%).
In this study percentage of prescribed vs. no prescribed drugs was high with diuretics (90.3% vs. 9.7%) and ACEIs (71% vs. 29%) and βB (83.4% vs. 16.6%) and low in valsartan/sacubitril (30.1% vs. 69.9%) and SGLT2i (34.1% vs. 65.9%) and MRA (38.7% vs. 61.3%) and this result resemble Peterklim study that resulted in ACEIs/ARBs (80%) βB (75%) MRA (62%) [11].
The low rate of ARNi (30.1%) and SGLT2i (34.1%) prescription indicate low implication of 2022 HF guideline in Yemeni patients in contrast of some consultants claim that they prefer to treat their patients as the guideline regardless to other factors (33.3%) of consultant however (60%) of them belief on that when applying guideline in Yemeni patients it will be clear improvement and the clinical trials showed the clear benefit in using SGLT2i and its recommended to use ARNI instead of ACEI.
Diuretics is recommended to HF patients who have fluid retention to relieve congestion and symptoms and to prevent worsening HF. Most patients with recent HF hospitalization require continued use of diuretics after discharge to prevent recurrent fluid retention and hospitalization but should be always used in combination with GDMT so it’s beneficial to use it as maintenance therapy in Yemeni patients in conjunction with GDMT and this study show it’s used in 90.3% of patients.
Telemedicine and telehealth are increasingly used for chronic management and remote monitoring a pragmatic randomized trial found that an initial telephone visit with a nurse or pharmacist to guide follow up reduce the need for in person visit; unfortunately, 63.1% of patients don’t have other than in person visit.
Education is recommended to patients with HF to optimize self-care and medications adherence and lifestyle change; it’s done by clarifying the goals of care in a rule “hope for the best plan for the worst” to share the medical decision making and increase the patient voice in clinical assessment and help the Yemeni patient to stop the cardiotoxic habits which is khat chewing, smoking and snuff use; snuff in its self is more cardiotoxic than smoking as shown in Robert study [12].
Education is important to encourage self-care furthermore self-management has been an important part of HF guideline for years. Patients should know the consequences of abrupt withdrawal of medications and nonadherence.
Consultants should use placebo for these objectives as seen in Karger study which resulted in chronic placebo therapy resulted in an 81 second improvement in exercise duration which was statistically significant when compared to pretreatment baseline and to the duration achieved by the non-placebo control group. Symptom improvement was seen in 71% of the participants, with an average improvement of 8.5%, P<0.05 [13].
Clinical pharmacist is a vital member of a multidisciplinary team in HF management to improve clinical outcomes and the one who is qualified to deal with medications issues and problems such as drug interactions and dose titration and follow up and to resolve financial burden of HF treatment so the clinical pharmacist has a critical rule in implicating GDMT and the majority (93.3%) of the physicians agreed on the importance of involving clinical pharmacist in HF management. Participation of a clinical pharmacist in ward/ICU rounds and clinical discussions helps to identify, prevent or reduce drug interactions and ADR. In addition to this, a clinical pharmacist can also actively participate in developing cost effective patient compliant therapy [14].
CONCLUSIONS
Guideline is the cornerstone in the treatment of HF and Yemeni patients need more help to benefit them form the guideline like more awareness and clinical pharmacist engagement in the treatment and telemedicine. There is a deviation between consultant treatment and the guideline. Further multi central researches are needed to highlight the importance of HF guideline in treating Yemeni patients with HF. According to the study results, the following recommendations are suggested:
•Implication of the recently guideline in treating Yemeni HF patients.
•A clinical pharmacist is qualified to optimize GDMT.
•Awareness the patients with more advice to be more adherent to medication and cessation of cardiotoxic habits.
•Consultant should use telemedicine for therapy monitoring and consultations.
•Diuretics should be used as continues in recurrent congestion and hospitalization only.
ETHICAL APPROVAL AND CONSENT TO PARTICIPATE
Full ethical clearance was obtained from the qualified authorities who approved the study design.
CONFLICT OF INTEREST
The authors have no conflicts of interest to declare.
References
- Hafkamp FJ, Tio RA, Otterspoor LC, et al. Heart Fail Rev. 2022;27(5):1683-1748.
[Crossref] [Google Scholar] [PubMed]
- Dassanayaka S, Jones SP. Circ Res. 2015;117(7):e58-e63.
[Crossref] [Google Scholar] [PubMed]
- Yancy CW, Jessup M, Bozkurt B, et al. J Am Coll Cardiol. 2013;128(16):1810-1852.
[Crossref] [Google Scholar] [PubMed]
- Roger VL. Epidemiology of heart failure. Circ Res. 2013;113(6):646-659.
[Crossref] [Google Scholar] [PubMed]
- Pfister R, Scholz M, Wielckens K, et al. Eur J Heart Fail. 2004;6(3):289-293.
[Crossref] [Google Scholar] [PubMed]
- Marti CN, Georgiopoulou VV, Kalogeropoulos AP. Curr Heart Fail Rep. 2013;10(4):427-433.
[Crossref] [Google Scholar] [PubMed]
- Tamargo J, Lopez-Sendon J. Nat Rev Drug Discov. 2011;10(7):536-555.
[Crossref] [Google Scholar] [PubMed]
- Members WC. J Card Fail. 2022;28(5):e1-e167.
- Harris H, Bromage DI, Dancy L, et al. Br J Gen Pract. 2019;69(683):313-314.
[Crossref] [Google Scholar] [PubMed]
- Steinman MA, Dimaano L, Peterson CA, et al. Med Care. 2013;51(10):901-907.
[Crossref] [Google Scholar] [PubMed]
- Peters-Klimm F, Müller-Tasch T, Remppis A, et al. J Eval Clin Pract. 2008;14(5):823-829.
[Crossref] [Google Scholar] [PubMed]
- Wolk R, Shamsuzzaman AS, Svatikova A, et al. J Am Coll Cardiol. 2005;45(6):910-914.
[Crossref] [Google Scholar] [PubMed]
- Archer TP, Leier CV. Cardiology. 1992;81(2-3):125-133.
[Crossref] [Google Scholar] [PubMed]
- Francis J, Abraham S. Saudi Pharm J. 2014;22(6):600-602.
[Crossref] [Google Scholar] [PubMed]